Eye Pressure Test Results: What Your Numbers Really Mean
The 3 AM Google Search Dilemma
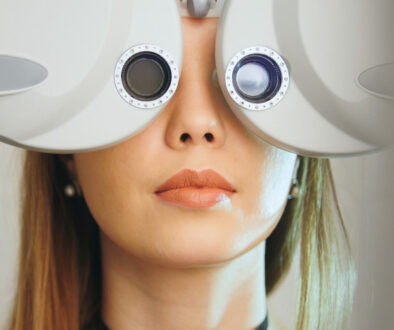
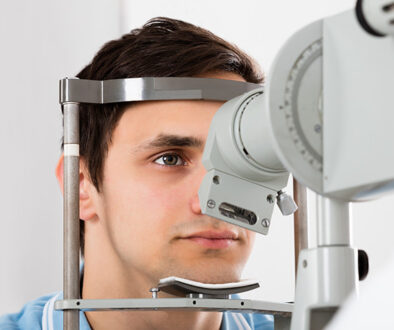
Your eye pressure test came back “high,” and now you’re staring at your phone at 3 AM, wondering if you’re going blind. The number 24 mmHg means nothing to you, but it sounds scary enough to keep you awake.
Here’s the reality: eye pressure numbers without context create unnecessary panic. What Richmond families really want to know isn’t just “what’s normal” – they want to understand what their specific results mean for their eyes, their family, and their future.
The difference between a reading and an interpretation is expertise. A chain store can measure your pressure in 30 seconds. Understanding what that measurement means for your individual risk requires knowledge, experience, and time – something you won’t get in a rushed screening.
At Frame & Focus Eye Care, Dr. Zaver believes no patient should leave confused about their results. Every number tells a story, but you need someone who speaks the language to translate it.
Questions about your results? Dr. Zaver explains every number.
Decoding Your Specific Numbers (Not Generic Ranges)
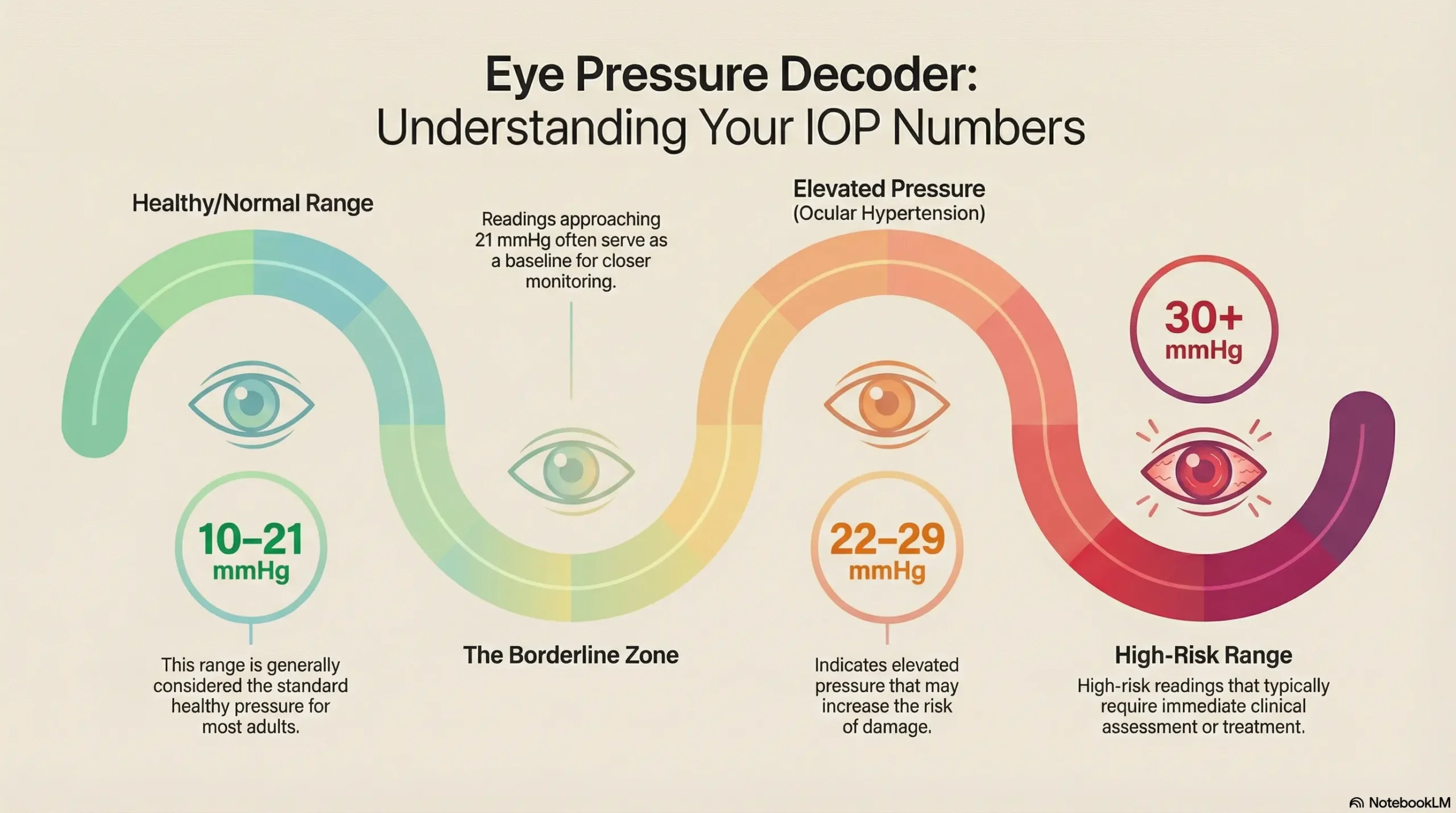
Normal eye pressure isn’t a one-size-fits-all number. While textbooks say 10-21 mmHg is “normal,” your personal baseline depends on factors most quick screenings ignore.
Why “Normal” Eye Pressure Isn’t the Same for Everyone
Your corneal thickness changes everything. Thick corneas can make pressure readings appear artificially high, while thin corneas can mask dangerous elevation. A reading of 22 mmHg might be perfectly safe for someone with thick corneas, but concerning for someone with thin ones.
Age matters more than most people realize. As you get older, your eye’s drainage system naturally becomes less efficient. A 25-year-old with a pressure of 18 mmHg faces different implications than a 65-year-old with the same reading.
Your Age, Ethnicity, and Family History: How They Change Your Numbers
African Americans develop glaucoma at younger ages and with lower pressures than other ethnic groups. Hispanic individuals show an increased risk after age 60. These aren’t statistics – they’re factors that should influence how your specific numbers are interpreted.
Family history doesn’t guarantee you’ll develop glaucoma, but it does change what pressure levels require monitoring. If your parent had glaucoma, a reading of 19 mmHg deserves more attention than it would for someone without genetic risk.
Richmond’s Climate and Seasonal Pressure Variations
Houston area heat and humidity affect eye pressure more than most people realize. Dehydration during summer months can temporarily elevate readings, while seasonal allergies common in our region can cause fluctuations that have nothing to do with glaucoma risk.
When 22 mmHg is Fine vs. When 18 mmHg Needs Attention
Context determines concern. A 22 mmHg reading in someone with thick corneas, no family history, and healthy optic nerves might require simple monitoring. An 18 mmHg reading in someone with thin corneas and a strong family history could signal the need for immediate treatment.
The key isn’t the number itself – it’s how that number fits into your complete eye health picture.
Ready for a thorough evaluation that explains exactly what your pressure readings mean for your long-term eye health? Dr. Zaver takes the time to discuss your results and create a personalized monitoring plan.
Beyond the Basic Reading: What Chain Stores Miss
Quick pressure checks miss critical factors that determine whether your numbers are truly concerning. Understanding why requires knowing what comprehensive testing actually includes.
Why Your Corneal Thickness Changes Everything
Most chain stores skip corneal pachymetry – the measurement that determines if your pressure reading is accurate. Without knowing your corneal thickness, pressure measurements are essentially guesswork.
Thick corneas (over 590 microns) can make your pressure appear 4-7 mmHg higher than it actually is. Thin corneas (under 520 microns) can hide dangerously high pressure by making readings appear deceptively low.
The Time-of-Day Factor Most Places Ignore
Eye pressure naturally peaks between 6 AM and 10 AM, then gradually decreases throughout the day. A reading of 25 mmHg at 8 AM might drop to 19 mmHg by 3 PM in the same person.
Chain stores typically see patients throughout the day without accounting for this variation. A comprehensive evaluation considers when your measurement was taken and how it fits into your daily pressure pattern.
Advanced Diagnostic Technology vs. Basic Screening Tools
Goldmann applanation tonometry – the gold standard for pressure measurement – requires skill and time. Many quick screenings use automated devices that provide approximate readings but lack the precision necessary for accurate diagnosis.
Frame & Focus uses multiple measurement techniques to ensure accuracy. If readings don’t align, additional testing determines which measurement reflects your true eye pressure.
How Dr. Zaver’s Comprehensive Approach Differs from Quick Checks
Comprehensive pressure evaluation includes corneal thickness measurement, multiple pressure readings, optic nerve assessment, and visual field testing when indicated. This process takes 15-20 minutes – not the 30 seconds typical of basic screenings.
Dr. Zaver explains not just what your pressure is, but why it measures that way and what it means for your specific situation. You’ll understand your results before leaving the office.
Experience advanced eye pressure testing with technology and expertise that provides accurate, reliable results you can trust.
The Borderline Zone: Your Next Steps Decision Tree
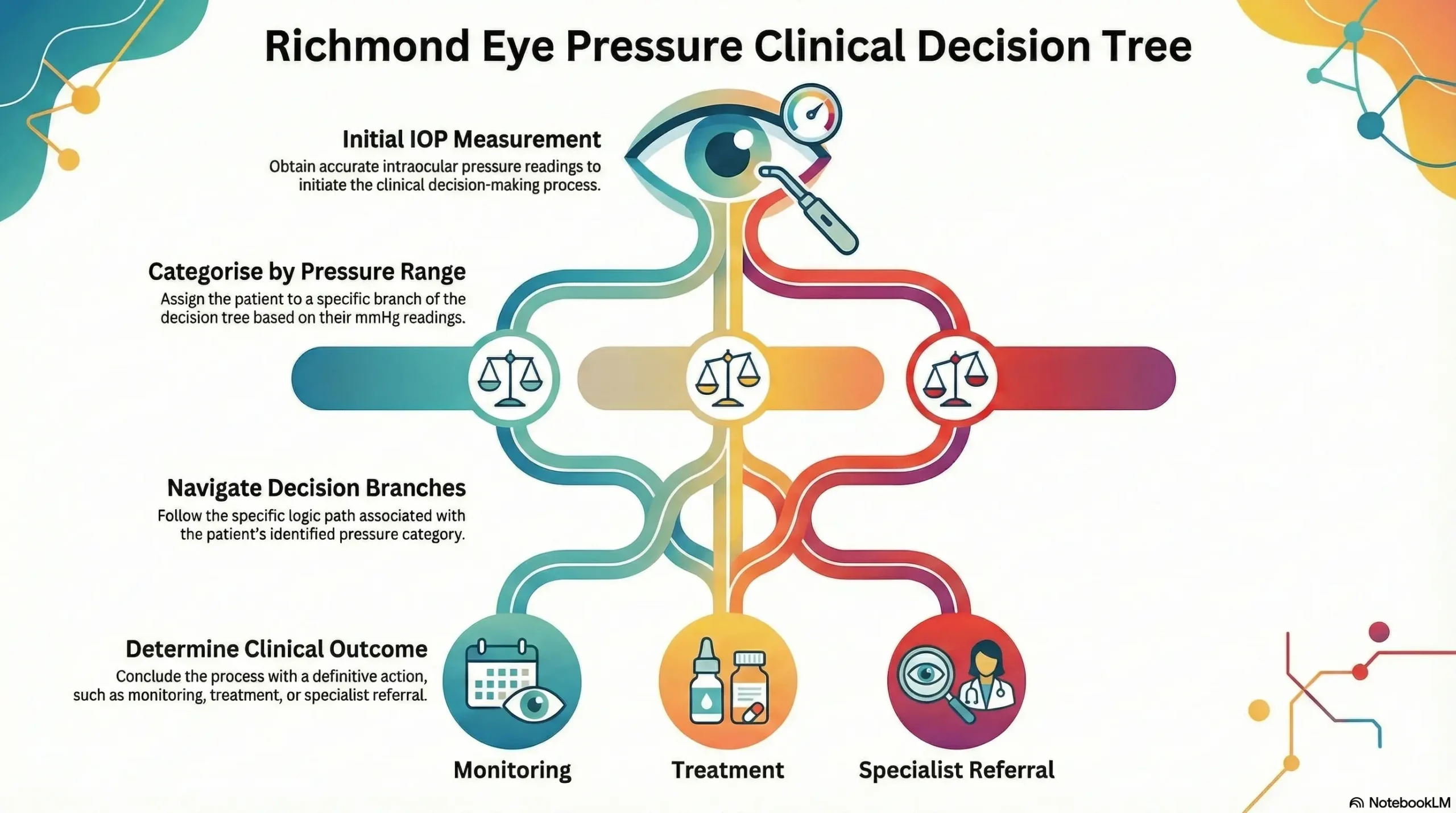
Borderline pressure readings (18-23 mmHg) leave many patients in limbo. Here’s how to navigate the next steps based on your specific situation.
What “Watch and Wait” Actually Means (And How Often to Check)
“Watch and wait” isn’t medical code for “ignore it.” It means establishing your personal pressure baseline through regular monitoring while watching for changes in your optic nerve and visual field.
Typical monitoring schedule:
- First 6 months: Every 3 months
- If stable: Every 6 months
- If family history or other risks: Every 3-4 months ongoing
When Borderline Results Require Immediate Action
Certain factors elevate borderline readings from “monitor” to “treat immediately”:
- Thin corneas (under 520 microns) with pressure over 20 mmHg
- Observable optic nerve damage
- Family history of aggressive glaucoma
- Pressure increase of 5+ mmHg from previous readings
The Richmond Advantage: No Referral Delays for Advanced Testing
Living in Richmond means access to a comprehensive glaucoma evaluation without driving to Houston Medical Center. Frame & Focus provides OCT imaging, visual field testing, and advanced pressure monitoring locally.
When a Houston specialist referral is necessary, Dr. Zaver coordinates care to ensure smooth transitions and continued local monitoring.
Building Your Personal Monitoring Schedule
Your monitoring plan depends on multiple factors:
- Low risk, stable pressure: Annual comprehensive exams
- Moderate risk: Every 6 months
- High risk or borderline readings: Every 3-4 months
- Treatment monitoring: Every 6-8 weeks initially
Dr. Zaver creates monitoring schedules that balance thorough care with practical convenience for Richmond-area families.
Create a personalized monitoring plan that gives you confidence in your eye health management.
Understanding Your Glaucoma Risk in Context
Family history creates anxiety, but understanding your actual risk helps separate realistic concern from unnecessary worry.
Why Family History Isn’t Destiny (But Requires Smart Planning)
Having a parent or sibling with glaucoma increases your risk 3-9 times, but this doesn’t mean you’ll definitely develop the disease. Many people with strong family histories never develop glaucoma with proper monitoring and early intervention when needed.
The key is understanding that family history changes your monitoring schedule and treatment thresholds – it doesn’t predetermine your outcome.
Normal Pressure Glaucoma: When “Good” Numbers Hide Problems
Approximately 30% of glaucoma patients have “normal” eye pressure (under 21 mmHg). This normal tension glaucoma proves that pressure is just one piece of the puzzle.
Signs that suggest normal pressure glaucoma:
- Progressive optic nerve changes despite normal pressure
- Visual field defects unexplained by other causes
- Strong family history with consistently normal pressure readings
Your Personal Risk Profile: Beyond Just the Pressure Reading
Complete risk assessment includes:
- Age: Risk doubles every decade after 40
- Ethnicity: African Americans are at higher risk starting at age 40
- Family history: Direct relatives with glaucoma
- Myopia: Nearsightedness increases risk
- Medical conditions: Diabetes, high blood pressure, sleep apnea
What Houston-Area Families Need to Know About Inherited Eye Disease
Regional genetic factors play a role in glaucoma patterns. The diverse population in the Houston metro area means varied genetic risk profiles that require individualized assessment.
Dr. Zaver considers your complete family history, not just glaucoma diagnoses. Relatives who went blind from “unknown causes” may have had undiagnosed glaucoma, especially in older generations when detection was less sophisticated.
Assess your complete glaucoma risk profile with a comprehensive evaluation that goes beyond family history to examine your individual factors.
The Second Opinion Decision: When and Where in Richmond
Knowing when to seek another evaluation protects your vision and provides peace of mind.
Red Flags That Require Another Evaluation
Seek immediate second opinion if:
- Pressure readings above 30 mmHg without a treatment plan
- Conflicting recommendations between providers
- Diagnosed with glaucoma, but felt rushed during evaluation
- Significant pressure increase (5+ mmHg) dismissed without explanation
- Treatment is recommended without a clear explanation of the necessity
Questions Your Current Provider Should Answer (But Maybe Didn’t)
Before leaving any eye pressure evaluation, you should understand:
- Your exact pressure readings and what they mean for you
- How your corneal thickness affects interpretation
- Your personal risk factors and monitoring schedule
- Why specific treatment is or isn’t recommended
- What changes would trigger treatment modifications
Why Frame & Focus Patients Never Leave with Unanswered Questions
Dr. Zaver’s approach ensures every patient understands their results before leaving. If you don’t understand something, the appointment isn’t over. This philosophy prevents the 3 AM Google searches that plague patients who receive numbers without explanation.
Second opinions are welcomed and encouraged when patients feel uncertain. Confidence in your eye care requires understanding, not blind trust.
When to Seek Houston Specialist Care vs. Comprehensive Local Testing
Houston Medical Center referral is appropriate for:
- Complex glaucoma requiring surgical intervention
- Unusual forms of glaucoma need subspecialist expertise
- Treatment failures requiring advanced intervention options
Richmond comprehensive testing handles:
- Pressure monitoring and interpretation
- Early glaucoma detection and treatment
- Routine glaucoma management
- Patient education and anxiety resolution
Concerned about your recent results or need immediate clarification? Dr. Zaver offers same-day consultations for urgent eye pressure concerns.
Local Resources & Citations
Fort Bend County Health Department: Provides community health screening information and referral resources for residents needing affordable eye care services throughout Richmond and the surrounding areas.
University of Texas Health Science Center at Houston: Offers comprehensive glaucoma research data and patient education materials, serving as a regional referral center for complex eye pressure management cases.
Texas Department of State Health Services: Maintains statewide vision health guidelines and screening recommendations, including protocols for eye pressure monitoring and glaucoma prevention programs.
American Academy of Ophthalmology: Provides evidence-based clinical guidelines for eye pressure evaluation and glaucoma management, establishing the medical standards followed by Richmond-area eye care professionals.
Your Eye Health Journey: From Results to Confidence
Understanding your eye pressure is just the beginning. Long-term eye health requires an ongoing partnership with someone who knows your history and watches for subtle changes.
What to Expect at Your Follow-Up Appointment
Comprehensive follow-up includes:
- Pressure measurement: Multiple readings using different techniques
- Comparison analysis: How today’s readings compare to your baseline
- Optic nerve photography: Documenting any changes since last visit
- Discussion time: Understanding what changes mean and why
How Frame & Focus Tracks Your Pressure Trends Over Time
Individual readings matter less than patterns. Dr. Zaver maintains detailed records showing how your pressure responds to different times of day, seasons, medications, and life changes.
This longitudinal tracking identifies subtle trends that single readings miss – like gradual increases that suggest the need for treatment or stable patterns that provide reassurance.
Building a Long-Term Eye Health Plan That Makes Sense
Your eye health plan evolves as you age and as your risk factors change. What starts as simple monitoring might eventually require treatment, or reassuring stability might allow for less frequent visits.
Dr. Zaver explains not just what’s happening now, but what to expect as you age and how your plan will adapt to changing circumstances.
Why Richmond Families Choose Continuity Over Convenience
Chain stores offer convenience but lack continuity. Having the same doctor who knows your history, understands your concerns, and recognizes subtle changes in your eyes provides security that quick screenings cannot match.
Frame & Focus builds relationships that span years, watching families’ eye health evolve and providing guidance tailored to each person’s unique situation and concerns.
Start your comprehensive eye health journey with a practice that treats every patient as an individual, not just a number.
FAQs
-
Normal eye pressure ranges from 10-21 mmHg, but your personal baseline matters more than generic ranges. Age, corneal thickness, and family history all influence what’s actually normal for your specific eyes. Regular monitoring helps establish your individual pattern rather than relying on population averages