Which Eye Drops Are Safe for Kids in Richmond?
Your child woke up with red, watery eyes — and now you’re standing in the pharmacy aisle staring at a wall of eye drop options, wondering which one is safe, which one actually works, and whether you even need drops at all. It’s a situation most parents in Richmond, Sugar Land, and Rosenberg have faced at least once.
Here’s the honest answer: not all eye drops are safe for children, and choosing the wrong one — even an over-the-counter product — can irritate a child’s developing eyes or mask a condition that needs proper treatment. This guide walks you through what you need to know before you reach for any bottle.
Why Children’s Eyes Are Different — and Why That Matters for Eye Drops
Children’s eyes are still maturing. The cornea, tear film, and ocular surface in kids are more sensitive to preservatives and active ingredients than adult eyes. What provides quick relief for a parent may cause stinging, toxicity, or a rebound reaction in a child.
This is especially relevant in the Richmond and Sugar Land area, where high humidity in summer shifts to dry indoor air in winter — both of which can trigger eye discomfort in kids who may not yet be able to explain exactly what they’re feeling.
The takeaway: always check the age labeling on any eye drop before use, and when in doubt, consult a pediatric eye doctor rather than guessing at the pharmacy.
The 4 Main Types of Eye Drops for Kids — and When Each Is Appropriate
Understanding the category of drop you’re dealing with is the first step to making a safe choice.
1. Preservative-Free Artificial Tears: These are the safest starting point for dry, irritated, or mildly red eyes in children. Products labeled “preservative-free” (often sold in single-use vials) avoid benzalkonium chloride (BAK), a common preservative that can irritate sensitive pediatric eyes with repeated use. Refresh Tears® in preservative-free form is one example frequently recommended by optometrists.
2. Antihistamine Eye Drops (Allergy) For children with seasonal allergies — very common in Fort Bend County during spring pollen season — antihistamine drops like Zaditor® (ketotifen) can relieve itching effectively. Most antihistamine drops are labeled for children 3 years and older. Always confirm age eligibility on the packaging.
3. Antibiotic Eye Drops (Prescription Only) Bacterial pink eye (conjunctivitis) requires prescription antibiotic drops. Parents should not attempt to treat suspected infections with leftover adult prescriptions or OTC redness-relief drops. Antibiotic drops such as Polytrim® are prescribed based on the child’s age and the specific bacteria involved — something only an eye exam can determine.
4. Steroid and Combination Drops (Prescription Only) These are not for OTC use. Steroid drops like FML (fluorometholone) are approved for children over age 3, but only under direct clinical supervision. Combination drops like Tobradex® (tobramycin and dexamethasone) are used when an infection and inflammation occur together. Self-medicating with steroid drops carries real risks, including elevated intraocular pressure in children.

Drops to Avoid in Children — Risks Most Parents Don’t Know About
Many products on pharmacy shelves are not appropriate for children, even though they’re easy to reach.
Redness-relief drops (vasoconstrictors) — products containing naphazoline or tetrahydrozoline, including some popular brands — are generally not recommended for children under 6, and some optometrists advise avoiding them for children altogether. These drops shrink blood vessels temporarily, but they don’t address the underlying cause and can cause a rebound effect where the eyes become even redder after the drops wear off.
Contact lens multipurpose solutions used as eye drops — this is a surprisingly common mistake. These solutions are not sterile for direct ocular use and can cause corneal irritation or abrasion in children.
Adult-formula drops without pediatric labeling — even some lubricating drops contain concentrations or preservatives calibrated for adult eyes. Always look for explicit age guidance on the label.
If your child is under 3 years old, the threshold should be clear: no OTC eye drops without direct guidance from an optometrist or pediatrician.
Houston-Area Allergies and Your Child’s Eyes: What’s Different Here
The Fort Bend County area has one of the highest year-round pollen loads in Texas. Mountain cedar in winter, oak and grass pollen in spring, and ragweed in fall create nearly continuous allergy seasons for many families in Richmond, Pecan Grove, and Fulshear.
For children with known seasonal allergies, itchy, watery eyes are often allergy-driven rather than infection-driven — an important distinction because the treatment approach differs completely. Antihistamine drops address the allergic response. Antibiotic drops do nothing for allergy symptoms.
The problem is that children often can’t distinguish between “my eyes are itchy and watery from allergies” and “my eyes hurt and have discharge from an infection.” A parent may confidently treat what looks like pink eye, when the underlying issue is allergic conjunctivitis — or the reverse.
If your child’s eye symptoms persist beyond 48 hours, or if there is yellow or green discharge, pain, or light sensitivity, that’s a signal for a professional exam rather than continued OTC management.
How to Apply Eye Drops to a Child — Without the Drama
Even the right drop won’t help if the application goes wrong. Here’s a practical approach that works for most children:
Have your child lie down on their back and tilt their head slightly toward the side of the affected eye. Gently pull down the lower eyelid to create a small pocket. Release one drop into that pocket — not directly onto the cornea. Ask your child to close their eyes gently (not squeeze), and wipe away any excess with a clean tissue. Avoid touching the dropper tip to the eye or eyelid to keep the bottle sterile.
For younger children who resist, some optometrists suggest having the child close their eyes while lying down, placing the drop in the inner corner of the eye, and then asking them to open their eyes — gravity does the rest.
Do not exceed the prescribed or labeled dosage. More drops does not mean faster relief, and overuse of certain drops can cause side effects.
When Eye Drops Are Not the Answer
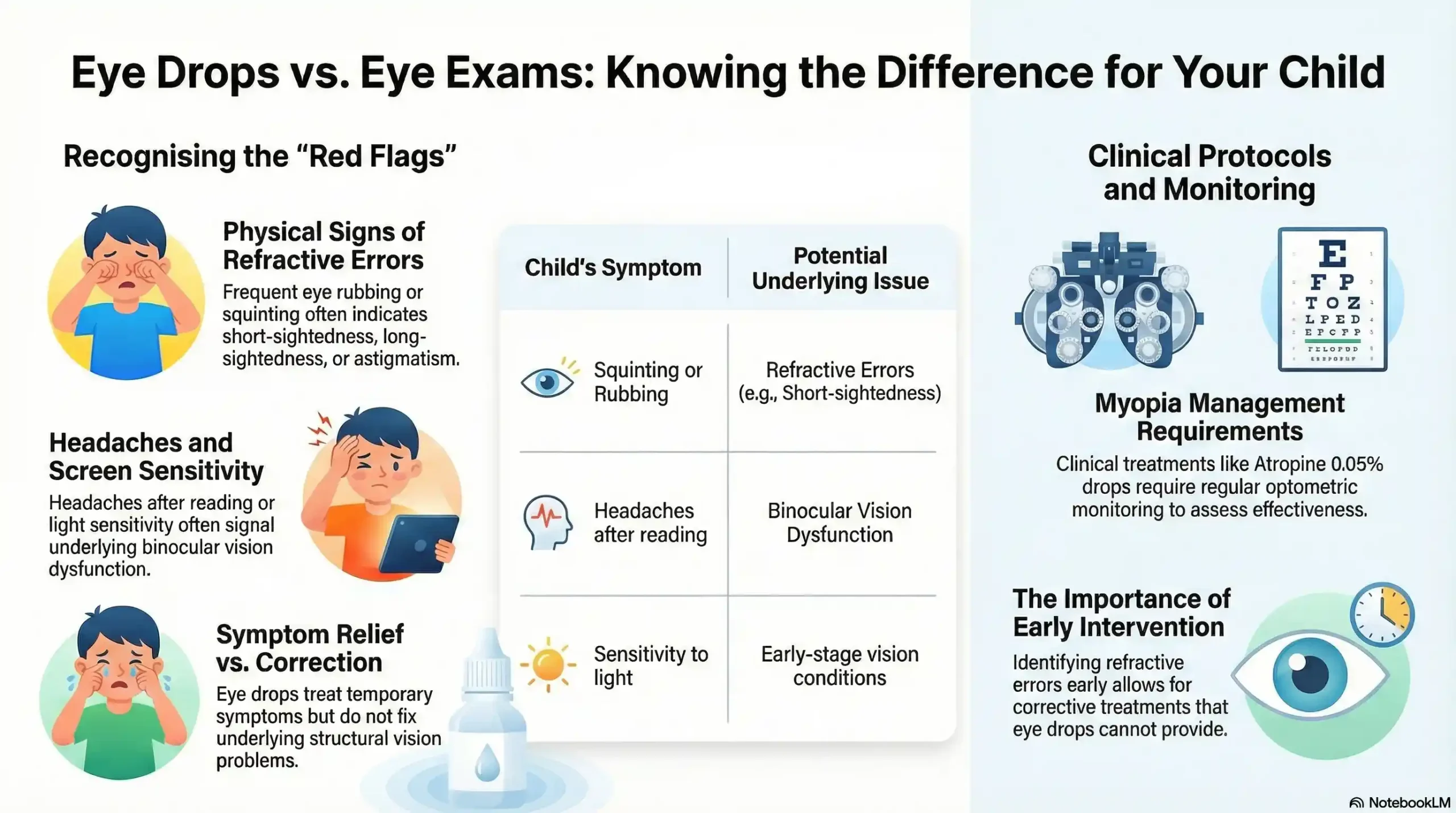
Eye drops treat symptoms. They don’t correct underlying vision problems, structural issues, or conditions that require a different approach.
If your child is rubbing their eyes frequently, squinting, complaining of headaches after reading or screen time, or showing signs of light sensitivity, these are not symptoms that any eye drop will resolve. These may point to refractive errors (nearsightedness, farsightedness, or astigmatism), binocular vision dysfunction, or early signs of conditions that benefit significantly from early intervention.
Similarly, if your child was prescribed atropine 0.05% drops for myopia management, that’s a clinical protocol — not a symptom treatment — and requires regular monitoring by an optometrist to assess effectiveness and adjust as needed.
Local Resources for Richmond, TX Parents
Fort Bend County Health & Human Services: Provides local health resources, immunization schedules, and referral information for pediatric healthcare in the Richmond area.
Texas DSHS – Children’s Vision Screening Requirements: Authoritative state guidance on vision screening requirements for school-age children in Texas — useful for knowing when your child is due for a mandated screening.
American Academy of Ophthalmology – Eye Drop Safety Guidelines: A reliable clinical reference for understanding which eye drop ingredients are considered safe for pediatric use.
MedlinePlus – Eye Care for Children (U.S. National Library of Medicine): Plain-language summaries of how common pediatric eye conditions and medications work, including dosage and safety considerations.
When It’s Time to See an Eye Doctor in Richmond, TX
Eye drops can be a useful tool — but they work best when they’re part of a clear diagnosis, not a first guess. If your child’s symptoms persist, worsen, or keep coming back, the most effective next step is a comprehensive pediatric eye exam.
At Frame & Focus Eye Care in Richmond, TX, Dr. Zaver and the team see patients from Richmond, Sugar Land, Rosenberg, Pecan Grove, and Fulshear. Same-day appointments are available for eye emergencies, and every exam includes a thorough discussion of what was found — in plain language, without jargon — so you can make an informed decision about your child’s care.
If you’re unsure whether your child’s eye symptoms need drops, glasses, or just a closer look, a pediatric eye exam at Frame & Focus is a practical starting point.
FAQs
-
Choose antihistamine drops like Zaditor or Pataday for children aged 2–3+. These provide fast, non-drowsy relief from itching and redness without using harsh vasoconstrictors that cause rebound irritation.