Eye Drop FAQs: Proper Use, Storage Tips & Common Mistakes
To use eye drops correctly, tilt your head back, pull down your lower eyelid, and instill one drop into the pocket formed. Close your eye gently for 60 seconds — do not blink hard. Store most drops in a cool, dry place and discard opened bottles after 28–30 days. The most common mistakes include touching the dropper tip to your eye, using expired drops, and skipping the wait time between multiple medications. When drops stop working or symptoms worsen, it is time to see a professional. Frame & Focus Eye Care in Richmond, TX — (832) 930-7797 — offers same-day appointments for urgent eye concerns.
Why Getting Eye Drops Right Actually Matters
There is a meaningful difference between using eye drops and using them correctly — and that difference has real clinical consequences.
Research consistently shows that improper instillation technique significantly reduces the amount of medication that actually reaches the eye. When you blink immediately after applying a drop, squeeze out two or three drops at once, or allow the bottle tip to graze your lash line, you are undermining the very treatment your doctor prescribed or you paid for at the pharmacy.
Beyond effectiveness, incorrect technique introduces contamination risks that can turn a routine medication routine into a genuine eye health threat. The good news is that with a few simple adjustments, most people can immediately improve both the safety and effectiveness of their eye drop routine.
The information below reflects what we teach our own patients at Frame & Focus Eye Care, guided by Dr. Sarah Zaver’s over a decade of clinical experience serving the Richmond and greater Houston area.
How to Properly Use Eye Drops — Step-by-Step
Proper instillation is a skill. Like any skill, it improves with intentional practice and the right technique. Here is exactly how to do it.
Before You Apply
Start with clean hands — always. Wash thoroughly with soap and water and dry completely before handling any eye drop bottle. This single step eliminates a significant source of contamination before the bottle even opens.
Next, check the expiration date printed on the bottle or box. Expired drops do not simply become less effective; in some formulations they can degrade into compounds that irritate or harm ocular tissue. If there is any doubt about whether a bottle is still within its usable window, discard it and open a fresh one.
Finally, if the instructions on your specific drops indicate shaking before use — particularly true for some suspension-based medications — do so. Not all drops require this step, but skipping it when required means you may be instilling an improperly mixed concentration.
The Correct Instillation Technique
Follow these steps precisely for effective, comfortable application every time:
- Tilt your head back slightly, or lie flat if that is more comfortable.
- Gently pull your lower eyelid downward with a clean fingertip to form a small pocket — this is called the conjunctival sac, and it is your target.
- Hold the bottle above your eye — close enough for accuracy, but far enough that the tip does not touch your eye, lashes, or skin. Approximately one inch is a safe distance.
- Squeeze gently to release exactly one drop into the pocket you created. One drop is the correct dose. The conjunctival sac holds approximately 7–10 microliters of fluid; a single eye drop contains around 50 microliters. Anything beyond one drop simply overflows — it does not increase therapeutic benefit.
- Close your eye gently. Do not squeeze or blink forcefully. Hard blinking pumps the medication out of the eye and down the nasolacrimal duct before it can be absorbed.
- Apply light pressure to the inner corner of your eye — the small area near the bridge of your nose — for approximately 60 seconds. This technique, called nasolacrimal occlusion, slows drainage and keeps the medication in contact with the ocular surface longer, significantly improving absorption.
If you miss the eye entirely, do not double-dose immediately. Wait a few minutes, reset your position, and try again calmly.
If You Wear Contact Lenses
Contact lens wearers have an additional layer of consideration that is frequently overlooked.
The vast majority of eye drops — including most prescription medications, antihistamines, and even many artificial tears — should not be applied while contact lenses are in place. The preservatives commonly found in eye drops can bind to soft contact lens material, concentrating on the lens surface and causing significant irritation over time.
The rule of thumb: remove your contacts before applying any drops unless the product is specifically labeled as safe for use with contacts. After applying your drops, wait a minimum of 15 minutes before reinserting your lenses to allow the medication to absorb and any preservative residue to clear.
The one widely recognized exception is rewetting or lubricating drops specifically formulated for use with contacts. These are a separate product category from standard artificial tears — check the label carefully before assuming they are interchangeable.
If you find yourself frequently relying on rewetting drops throughout the day, that is not a minor inconvenience to manage with more drops. It is a clinical signal worth investigating.
📌 Struggling with dry, irritated eyes even while wearing contacts? The solution may not be another bottle — it may be the right lens altogether. At Frame & Focus Eye Care, our Specialty Contact Lens Fitting service is designed to find the precise fit and material that works with your eyes, not against them. Call (832) 930-7797 to schedule your fitting today.
Eye Drop Storage — What You’re Probably Doing Wrong
Correct storage is just as important as correct application — yet it is the step most patients never think about until something goes wrong.
Room Temperature vs. Refrigeration
Most over-the-counter eye drops are formulated to be stored at room temperature, in a cool and dry location away from direct sunlight. The critical word here is dry — which immediately disqualifies the most popular storage spot in most households.
The bathroom medicine cabinet, despite its name, is one of the worst places to store eye drops or any medication. The heat and humidity generated by daily showers create an environment that degrades preservatives, accelerates bacterial growth, and compromises the stability of active ingredients faster than most people realize.
A bedroom nightstand drawer, a kitchen cabinet away from the stove, or a dedicated medication shelf in a cool room are all significantly better options.
For prescription eye drops, always defer to the specific storage instructions on your label. Some formulations — particularly certain glaucoma medications and compounded drops — do require refrigeration. Do not assume. Read the label and confirm with your pharmacist or with Dr. Zaver at your next visit.
How Long Are Eye Drops Good After Opening?
This is one of the most common questions we receive at Frame & Focus Eye Care — and the answer surprises most patients.
Multi-dose bottles of preserved eye drops should generally be discarded 28 to 30 days after opening, regardless of how much product remains in the bottle. Once a multi-dose bottle is opened, the preservative system that prevents bacterial growth begins to deplete with every use. By day 30, that protection may no longer be adequate — even if the drops look and feel completely normal.
Preservative-free drops, which typically come in small single-use vials, are designed for one-time application. Once you open a vial and use it, discard it. These formulations contain no preservative at all, meaning bacterial contamination can begin immediately upon exposure to air.
Prescription eye drops vary by formulation. Follow your prescribing doctor’s specific instructions, and when in doubt, call our office at (832) 930-7797 — we are happy to clarify.
A practical habit worth building: write the date you opened each bottle on the label with a permanent marker. It takes three seconds and eliminates the guesswork entirely.
The Dropper Tip — Your Biggest Contamination Risk
The dropper tip is the most overlooked component of eye drop safety, and it is where contamination most frequently originates.
The tip of your eye drop bottle must never make contact with any surface — not your eye, not your eyelid, not your finger, and not the countertop you set it down on. Each point of contact introduces microorganisms that can multiply inside the bottle between uses, transforming a sterile medication into a potential source of infection.
After every use, replace the cap securely and promptly. If you notice that your drops have become cloudy, discolored, or have developed visible particles — stop using them immediately and replace the bottle, even if it is not yet 30 days old.
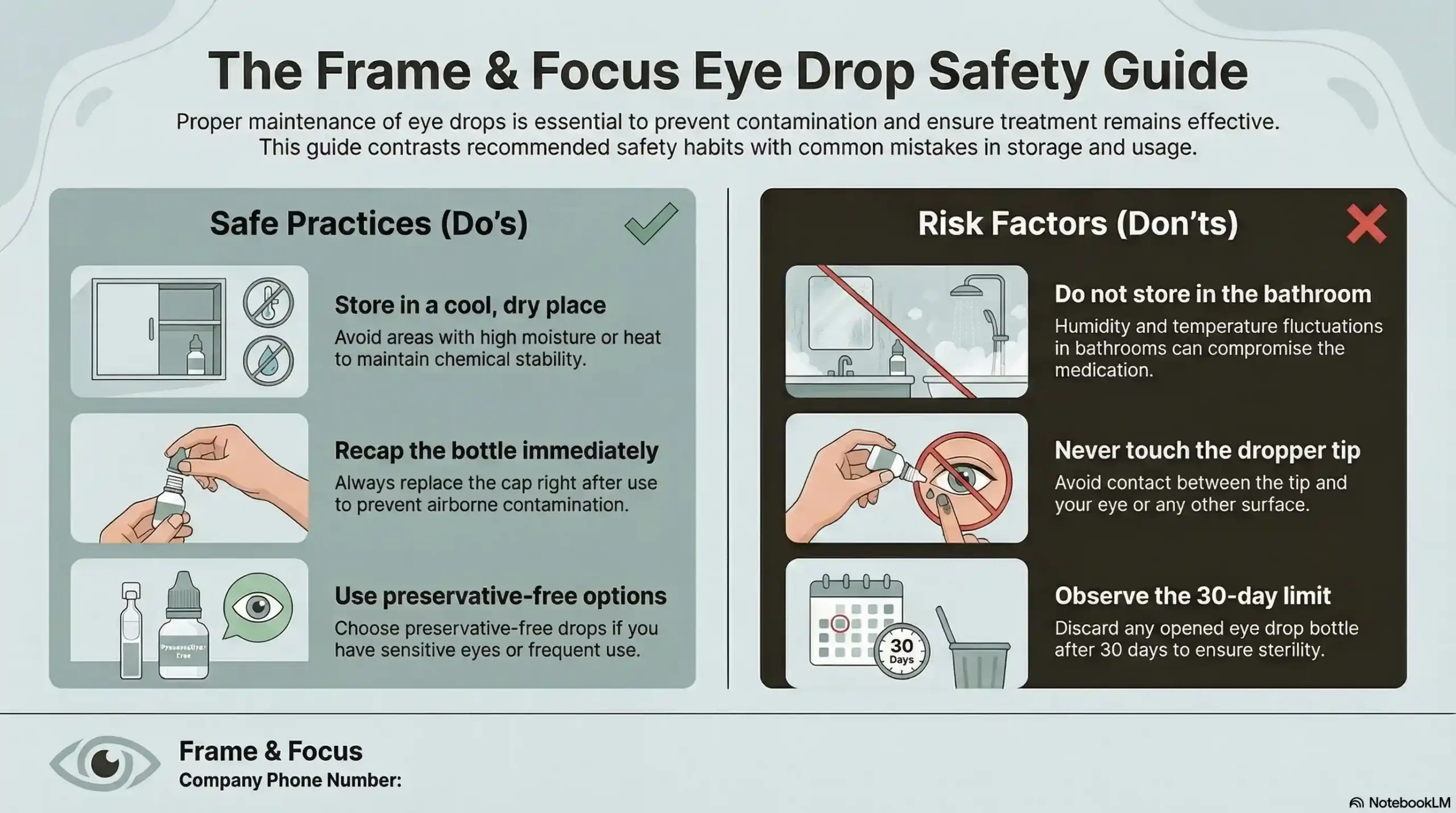
| Category | ✅ Do’s | ❌ Don’ts |
|---|---|---|
| Storage Location | Cool, dry place away from sunlight | Bathroom cabinet — heat and humidity degrade drops |
| Temperature | Follow label instructions precisely | Leave in a hot car or on a sunny windowsill |
| After Opening | Write date on bottle; discard at 28–30 days | Continue using past the open-date window |
| Dropper Tip | Recap securely and immediately after use | Allow tip to touch eye, skin, lashes, or surfaces |
| Sharing | Keep your drops personal to you | Share bottles with family members |
| Preservative-Free Vials | Use the entire vial in one session | Save and reuse an opened single-use vial |
The 7 Most Common Eye Drop Mistakes
Even patients who have been using eye drops for years are often making at least one of these mistakes. Here are the most common errors we see — and exactly how to correct them.
1. Touching the dropper tip to your eye or skin. This is the single most dangerous and most common mistake. It directly contaminates your bottle and creates a vehicle for introducing bacteria into your eye with every subsequent use. Always maintain at least one inch of clearance between tip and eye.
2. Using expired drops. Expired drops are not just ineffective — some degraded formulations can actively irritate ocular tissue. Check dates at every refill of your medicine cabinet and replace bottles that have passed their expiration or their 30-day open window.
3. Applying more than one drop. More is not more when it comes to eye drops. The eye simply cannot hold the volume of multiple drops simultaneously. Excess medication spills onto your cheek, is absorbed through the skin, or drains into the nasal passage where it can enter the bloodstream — increasing systemic exposure without any additional therapeutic benefit.
4. Blinking hard immediately after instillation. Hard blinking is the reflex that pumps fluid out of the eye. Do it right after applying drops and you have effectively ejected a significant portion of your medication. Close gently, apply inner-corner pressure, and let the drop absorb.
5. Applying drops in the wrong order when using multiple medications. If you use more than one type of eye drop, order matters. The general clinical rule is thinnest consistency first, thickest last. Thicker formulations like gels create a barrier that prevents subsequent drops from penetrating adequately. Always apply standard drops before gels, and gels before ointments.
6. Skipping doses of prescription drops — especially glaucoma medications. Glaucoma medications work by maintaining consistent intraocular pressure control. Skipping doses allows pressure to fluctuate, which can cause progressive, irreversible optic nerve damage that patients often cannot feel happening. Consistency is not optional with glaucoma therapy.
7. Using OTC drops to manage symptoms that require professional diagnosis. This is perhaps the most consequential mistake on this list. Over-the-counter artificial tears, antihistamines, and redness-relieving drops are appropriate for mild, temporary symptoms. When those same symptoms persist, worsen, or keep returning — using more OTC drops is not treatment. It is delay. It masks the signal your eye is sending and allows underlying conditions to progress undetected.
Using Multiple Eye Drops — The Timing Rules You Need to Know
Many of our patients in Richmond and Sugar Land manage more than one eye condition simultaneously, which means more than one bottle of drops. The interaction between those drops — and the timing of their application — matters more than most people realize.
The 5-Minute Rule
When using two or more different eye drop medications, always wait a minimum of five minutes between each application. This interval is not arbitrary. It allows the first drop to absorb adequately before the second drop dilutes it, washes it out, or competes for the same receptor sites on the ocular surface.
Applying two drops back to back with no wait time is one of the most common reasons prescription eye drops underperform — the patient is compliant, but the medications are interfering with each other.
The Correct Application Order
Follow this sequence whenever you are using multiple drop types:
- Standard liquid drops first — antihistamines, antibiotics, glaucoma medications, and standard artificial tears
- Eye gels second — lubricating gels that have a thicker, more viscous consistency
- Eye ointments last — always reserved for bedtime due to temporary blurring of vision
Thicker formulations create a film over the ocular surface that physically blocks thinner drops from penetrating. Getting the order right ensures each medication reaches its target at adequate concentration.
Prescription and OTC Combinations
Never assume that over-the-counter and prescription drops are safe to combine without your doctor’s knowledge. Both categories can contain preservatives, vasoconstrictors, and active ingredients that may interact — reducing effectiveness or, in some cases, producing unintended side effects.
At every appointment at Frame & Focus Eye Care, Dr. Zaver reviews all eye drops — prescription and OTC — as part of a complete picture of your ocular health. If you have started a new OTC product between visits, bring the bottle or note the name. That information matters.
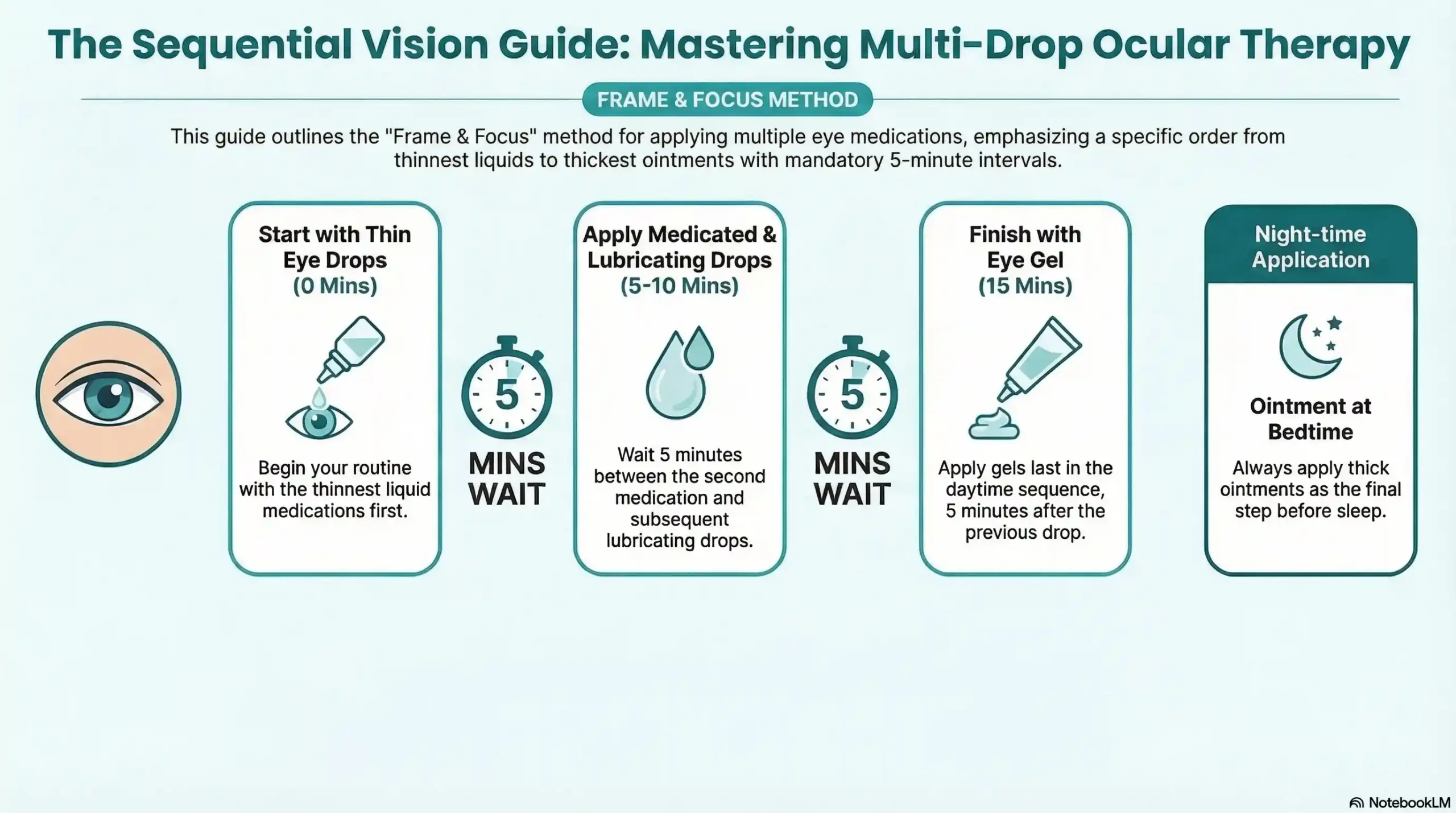
| Application Step | Product Type | Minimum Wait After |
|---|---|---|
| Step 1 | Thin medicated drops (antihistamine, antibiotic, glaucoma) | 5 minutes |
| Step 2 | Second prescribed medication if applicable | 5 minutes |
| Step 3 | Standard artificial tears / lubricating drops | 5 minutes |
| Step 4 | Thicker lubricating gel | 5 minutes |
| Step 5 | Eye ointment | Apply at bedtime only |
When Eye Drops Aren’t Enough — Signs You Need to See a Doctor
Eye drops — even the best ones, used perfectly — are not a solution for every eye condition. Knowing when drops are appropriate and when they are a substitute for care you actually need is one of the most important pieces of eye health literacy we can offer.
See an eye doctor promptly if you are experiencing any of the following, even if you are currently using drops:
- Persistent redness that does not resolve within 48–72 hours — this is not a “more drops” situation
- Pain inside the eye — distinct from surface irritation, this warrants urgent evaluation
- Sudden changes in vision — blurring, halos, loss of peripheral vision, or flashes of light
- Sensitivity to light that is new or worsening
- Discharge that is yellow, green, or crusted — signs of infection that require prescription treatment, not OTC management
- A foreign body sensation that does not clear after rinsing with sterile saline
For patients with chronic dry eye specifically: if you are using artificial tears more than four times per day and still experiencing significant symptoms, your dry eye likely has an underlying cause — meibomian gland dysfunction, an autoimmune component, or a medication side effect — that artificial tears are not designed to address. Targeted Dry Eye Treatment, like what we offer at Frame & Focus Eye Care, is built for exactly this situation.
We also offer same-day emergency appointments for urgent eye concerns. You should never have to decide between waiting days for care and driving to an urgent care center staffed by providers without specialized eye training. When something is wrong with your vision, a local eye doctor is always the right call.
📌 Your eyes are telling you something — and drops alone may not be the answer. At Frame & Focus Eye Care, our Dry Eye Treatment goes beyond symptom management to identify and treat root causes. Call (832) 930-7797 today. Same-day appointments are available for urgent needs.
A Note for Parents — Eye Drops for Children
Children and eye drops are a notoriously difficult combination — and yet pediatric eye drop use is more common than most parents expect, spanning allergy management, amblyopia treatment, infection care, and myopia management protocols.
A few practical realities worth knowing:
Resistance is normal and manageable. For young children, the “closed eye” technique — applying the drop to the inner corner of the closed eye while the child lies flat, then asking them to open their eye — allows the drop to passively enter without the instinctive flinching that makes standard application difficult.
Adult drops are not automatically appropriate for children. Always confirm with Dr. Zaver or your child’s prescribing physician that a specific formulation is appropriate for your child’s age and weight before use. Dosing and preservative considerations differ meaningfully between pediatric and adult populations.
Frequent eye rubbing or complaints of blurry vision in a school-age child are not always an allergy. They can be signals of myopia progression — nearsightedness that worsens throughout childhood if not proactively managed. Frame & Focus Eye Care offers Myopia Management services specifically designed to slow the progression of nearsightedness in children, offering their developing eyes a better long-term trajectory than glasses alone can provide.
If your child has been struggling in school, avoiding reading, or complaining of headaches, an eye exam at Frame & Focus Eye Care is a worthwhile first step — before assuming the cause is behavioral or developmental.
🏛️ Local Resources & Citations
1. U.S. Food & Drug Administration (FDA) — Eye Drop Safety & Contamination Warnings (Government — .gov) The FDA actively monitors and issues public alerts on contaminated, counterfeit, and improperly packaged eye drops — check here to verify whether any drops you are using have been flagged for safety recalls or contamination warnings before your next use.
2. Texas Health & Human Services — BEST Program (Blindness Education, Screening & Treatment) (Government — .gov | State of Texas) Texas residents may be eligible for free vision screenings and financial assistance for medically urgent eye treatment through this state-funded program — Richmond and Fort Bend County residents without insurance coverage can use BEST as a pathway to professional eye care when OTC drops are no longer sufficient.
3. Fort Bend County Health & Human Services — Assistance Through Other Agencies (Government — .gov | Fort Bend County) Fort Bend County’s indigent health care program lists local and regional eye care assistance resources for residents, including the University Eye Institute’s Eye Care Assistance Program — a practical first stop for Richmond-area patients who need professional eye care guidance beyond what a pharmacy bottle can provide.
4. University of Houston College of Optometry — UH Health Eye Care (Educational — .edu | Closest accredited optometry institution to Richmond, TX) The only public optometry training program in Texas, serving more than 50,000 patients annually, UH Health Eye Care is the nearest accredited academic eye care center to the Richmond area — a credible regional resource for patients seeking advanced dry eye, specialty contact lens, or disease management services beyond routine care.
Your Richmond Eye Care Partner — Frame & Focus Eye Care
At Frame & Focus Eye Care, we were built on a single belief: every patient deserves care that goes beyond a transaction. That means thorough exams, honest communication, and a team that treats you like family — because in our practice, that is not a marketing phrase. It is how we show up every single day.
Dr. Sarah Zaver brings over a decade of experience serving the Richmond and greater Houston area, with a clinical reputation built on being patient, thorough, and genuinely passionate about eye health outcomes. Our team has earned a 4.9-star rating across 315 Google reviews through consistent, compassionate, detail-oriented care.
We proudly serve patients across Richmond, Pecan Grove, Sugar Land, Rosenberg, and Fulshear with a full suite of services, including:
- Comprehensive Eye Exams
- Dry Eye Treatment
- Specialty Contact Lens Fittings
- Myopia Management
- Emergency Eye Care
- Quality Eyewear including our $99 Frame Special
We are open Monday through Thursday from 10:00 AM to 6:00 PM and Friday from 10:00 AM to 4:00 PM. Same-day appointments are available for urgent needs.
📌 You deserve an eye care partner who speaks plainly, listens carefully, and genuinely puts your health first. Schedule your appointment with Frame & Focus Eye Care today.
📍 18310 W Airport Blvd #900, Richmond, TX 77407
📞 (832) 930-7797
Book online or call — we look forward to seeing you.
Frequently Asked Questions
-
To properly put in eye drops, tilt your head back, gently pull your lower eyelid down to form a small pocket, and hold the bottle tip approximately one inch above your eye. Release exactly one drop into the pocket, close your eye gently without blinking hard, and apply light pressure to the inner corner for 60 seconds to maximize absorption. Wash your hands thoroughly before starting.