Can Diet Reverse Diabetic Retinopathy
While a healthy diet and stable A1c levels are vital for managing diabetes, diet alone cannot reverse existing structural damage to the retina caused by diabetic retinopathy. However, specific nutritional strategies—such as flattening glucose spikes and increasing anti-angiogenic foods—can stop the progression of the disease and protect your remaining vision. At Frame & Focus Eye Care, Dr. Sarah Zaver combines these lifestyle interventions with advanced retinal imaging to manage your eye health with clinical precision
Why Your A1c Isn’t the Full Story: The Spike Factor
Many patients feel frustrated when their A1c is within a “normal” range, yet their retinopathy continues to progress. The missing piece of the puzzle is often glycemic variability.
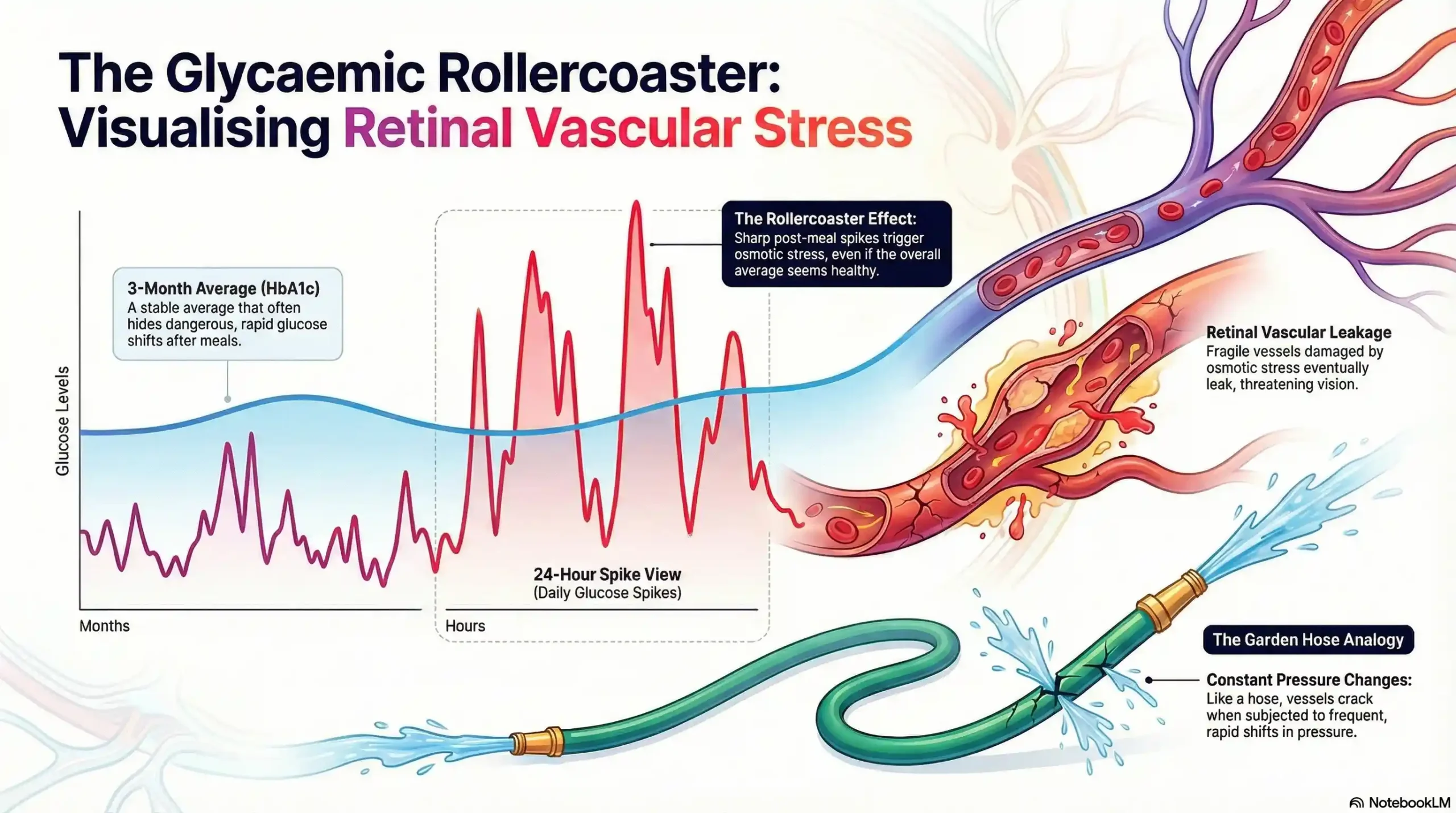
While your A1c is a three-month average, it can hide sharp glucose “spikes” that occur after meals. Research in JAMA Ophthalmology suggests these rapid shifts cause osmotic stress, making fragile retinal vessels more likely to leak.
-
The “Rollercoaster” Effect: Think of your blood vessels like a garden hose; constant pressure changes eventually cause cracks.
-
The Solution: Focus on “flattening the curve.” Pair your carbohydrates with proteins and healthy fats to slow sugar absorption.
-
Expert Tip: During a comprehensive eye exam, we use advanced retinal photography to see if these spikes are causing “silent” damage before you even notice vision changes.
Schedule Your Proactive Diabetic Eye Exam in Richmond
The “Anti-Angiogenic” Kitchen: Starving Abnormal Vessels
In advanced diabetic retinopathy, the eye attempts to fix itself by growing new, weak blood vessels (neovascularization). These vessels are prone to bleeding and can cause vision loss. Modern medicine treats this with “Anti-VEGF” injections, but you can support this process in your kitchen.
-
Green Tea (EGCG): Contains powerful catechins that may help inhibit the signals that trigger abnormal vessel growth.
-
Cruciferous Vegetables: Broccoli and kale are rich in sulforaphane, which activates the Nrf2 pathway—your body’s internal shield against retinal oxidative stress.
-
Omega-3s: Found in salmon and flaxseeds, these “good fats” are essential for maintaining the structure of your retina.
Intermittent Fasting and Retinal “Recycling”
Can skipping a late-night snack save your sight? Emerging research from the American Diabetes Association (ADA) suggests that “Time-Restricted Feeding” may trigger a process called autophagy.
-
What is Autophagy? Think of it as your retina’s internal “recycling program.” It is the process where your cells clear out damaged proteins and debris.
-
The Connection: By giving your body a break from constant digestion, you allow your cellular “clean-up crews” to focus on repairing damaged tissues.
-
Safety First: If you are managing diabetes, always coordinate fasting with your primary doctor. If you notice sudden vision changes like new floaters during a lifestyle shift, contact us for emergency eye care immediately.
Treatment
While a healthy diet and exercise can be beneficial to your optical health, diabetic retinopathy is a condition that is caused by damage to the retinal wall. While this damage can sometimes be corrected, simple diet changes won’t reverse the effects.
It is essential to catch the condition in the earlier stages to reduce the effects. This can also help patients understand the importance of monitoring their blood sugar so that repeat events can be limited. Treatment options are even more successful when diabetic retinopathy is caught early. These options include vitrectomy, scatter photocoagulation, and focal photocoagulation.
During both scatter and focal photocoagulation, the doctor will use lasers to help alleviate the condition. The lasers make small burns on the retina aimed at the blood vessels. These burns will help to seal the blood vessels to prevent more leakage and stop them from growing larger.
When using scatter photocoagulation, hundreds of small burns are made in a specific pattern during two additional appointments. Scatter coagulation should be used on patients who do not have advanced diabetic retinopathy.
Focal photocoagulation specifically targets the leaking blood vessels that are in the macula. Unfortunately, this procedure is not aimed at correcting the blurry vision associated with diabetic retinopathy, but it does stop it from progressing further. Once the retina has detached, neither form of photocoagulation can be used.
Vitrectomy is a surgery that helps to remove scar tissue and/or the fluid that is clouded with blood that has leaked into the eye. This operation is the most successful when performed before the disease has progressed too far. When the operation only targets removing the fluid, success rates are very high for the procedure. When the procedure also aims to reattach the retina, the failure rate is around 50%.
Living with Retinopathy
Retinopathy affects every person and even the same pair of eyes differently. A one-size-fits-all approach isn’t possible, and it is important to talk to your medical professional about which options or treatment plans are right for you.
The Gut-Eye Axis: Your Microbiome and Your Vision
The health of your gut directly influences the level of inflammation in your eyes. A “leaky gut” can lead to systemic inflammation that weakens the blood-retinal barrier.
-
The Fiber Factor: Foods like lentils and whole grains produce butyrate in the gut, which acts as a natural anti-inflammatory for your eyes.
-
Probiotic Protection: Fermented foods like kimchi or unsweetened yogurt help balance your microbiome, potentially reducing the inflammatory markers linked to retinopathy.
-
The Big Picture: Systemic inflammation affects more than just your retina. If you find that eye inflammation is causing chronic headaches or discomfort, learn how Neurolens technology can help realign your vision and restore comfort.
Resources and Citations
American Diabetes Association Standards of Care in Diabetes—2024
Retinopathy, Neuropathy, and Foot Care Guidelines
The American Diabetes Association’s 2024 Standards of Care provides the most current clinical practice recommendations for diabetic retinopathy screening, prevention, and management. This authoritative source confirms that diabetic retinopathy is the most frequent cause of new cases of blindness among adults aged 20–74 years in developed countries, emphasising the critical importance of early detection and proactive care. The guidelines detail evidence-based screening schedules and treatment protocols that eye care professionals use to protect patients’ vision.
Journal of the American Medical Association Ophthalmology: Current U.S. Prevalence Data
Prevalence of Diabetic Retinopathy in the US in 2021
This landmark study provides the most recent comprehensive analysis of diabetic retinopathy prevalence across the United States. The research estimates that 9.60 million people in the US (26.43% of those with diabetes) had diabetic retinopathy and 1.84 million people (5.06% of those with diabetes) had vision-threatening diabetic retinopathy in 2021. This data underscores the substantial public health impact of diabetic retinopathy and demonstrates why regular eye examinations are essential for all individuals living with diabetes.
It’s important to continue to learn about how you can manage diabetes to help keep the progression of diabetic retinopathy at bay. Make sure to use the tools that are available to you. Test your blood glucose daily, schedule your regular doctor appointments and annual exams, and learn to listen to your body. We can often start to detect that something is going on when things just don’t feel right.
Managing your diabetes with a sudden vision loss can lead to an increase in the quality of life and help to stop further vision loss.
Take Control of Your Vision Today
Managing diabetic retinopathy requires more than just diet—it requires a partner in your long-term health. At Frame & Focus Eye Care, Dr. Sarah Zaver uses advanced retinal photography to monitor your eye health with clinical precision and “Straight Talk” clarity.
Don’t wait for your vision to change. Schedule your proactive Diabetic Eye Exam in Richmond today, and let’s build your personalized vision roadmap together.
FAQs
-
No. While diet is crucial for control, professional treatment (like laser or injections) and strict blood glucose management are necessary to stop progression and potentially improve early damage.